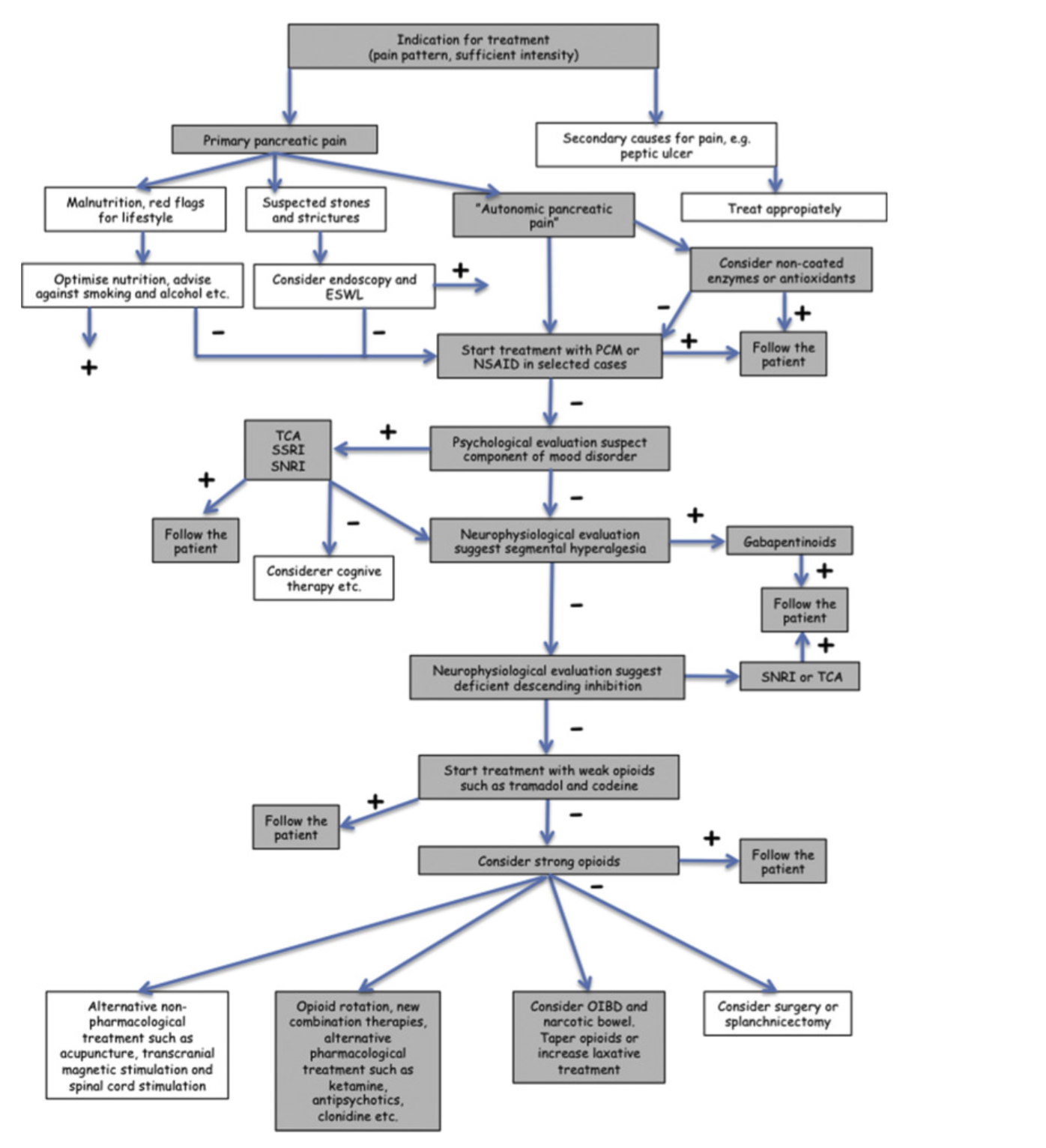
Pain Management In Pancreatitis. Analgesics are administered for pain relief. Both pain intensity and the frequency of pain attacks have been shown to. The experimental measures have been shown to be effective in numerous studies with murine or porcine ap models yet have not been translated into clinical. Chronic pancreatitis cp is a poorly understood disease to the immense frustration of patients clinicians and researchers.

The experimental measures have been shown to be effective in numerous studies with murine or porcine ap models yet have not been translated into clinical. Opioids may be needed for effective pain control. The risks measurements of severity and management of severe acute pancreatitis and its complications have evolved rapidly over the past decade. The aetiology of chronic pancreatitis cannot be determined from the pain profile but painless courses of the disease are rare in alcoholic chronic pancreatitis 10 of cases whereas the painless state is more frequent in the late onset type of idiopathic chronic pancreatitis and in tropical chronic pancreatitis. Abdominal pain is the foremost complication of chronic pancreatitis cp. Antibiotics are generally not indicated.
In most patients the disease takes a mild course where moderate fluid resuscitation management of pain and nausea and early oral feeding result in rapid clinical improvement.
Use a pain score to monitor the response to analgesia and adjust the dose and or type of analgesic using local pain management protocols. Acute pancreatitis is an inflammatory condition of the pancreas most commonly caused by bile stones or excessive use of alcohol. There is good news. Both pain intensity and the frequency of pain attacks have been shown to. Use a pain score to monitor the response to analgesia and adjust the dose and or type of analgesic using local pain management protocols. Antibiotics are generally not indicated.